Can brain hemorrhage be cured?
Recovery from a brain hemorrhage is possible in many cases, especially with rapid medical intervention and a carefully planned treatment approach. The extent of recovery depends on several key factors that directly affect healing outcomes, such as the size of the hemorrhage, its location in the brain, the patient’s age, and overall health condition.
Outcomes vary from one patient to another. Some cases show gradual improvement with near-complete restoration of neurological functions, while others may experience permanent complications requiring long-term rehabilitation.
In this article, we will review the factors affecting recovery, the main treatment options available, and the steps that can be taken to support healing and safely improve the chances of regaining health.
Brain Hemorrhage:
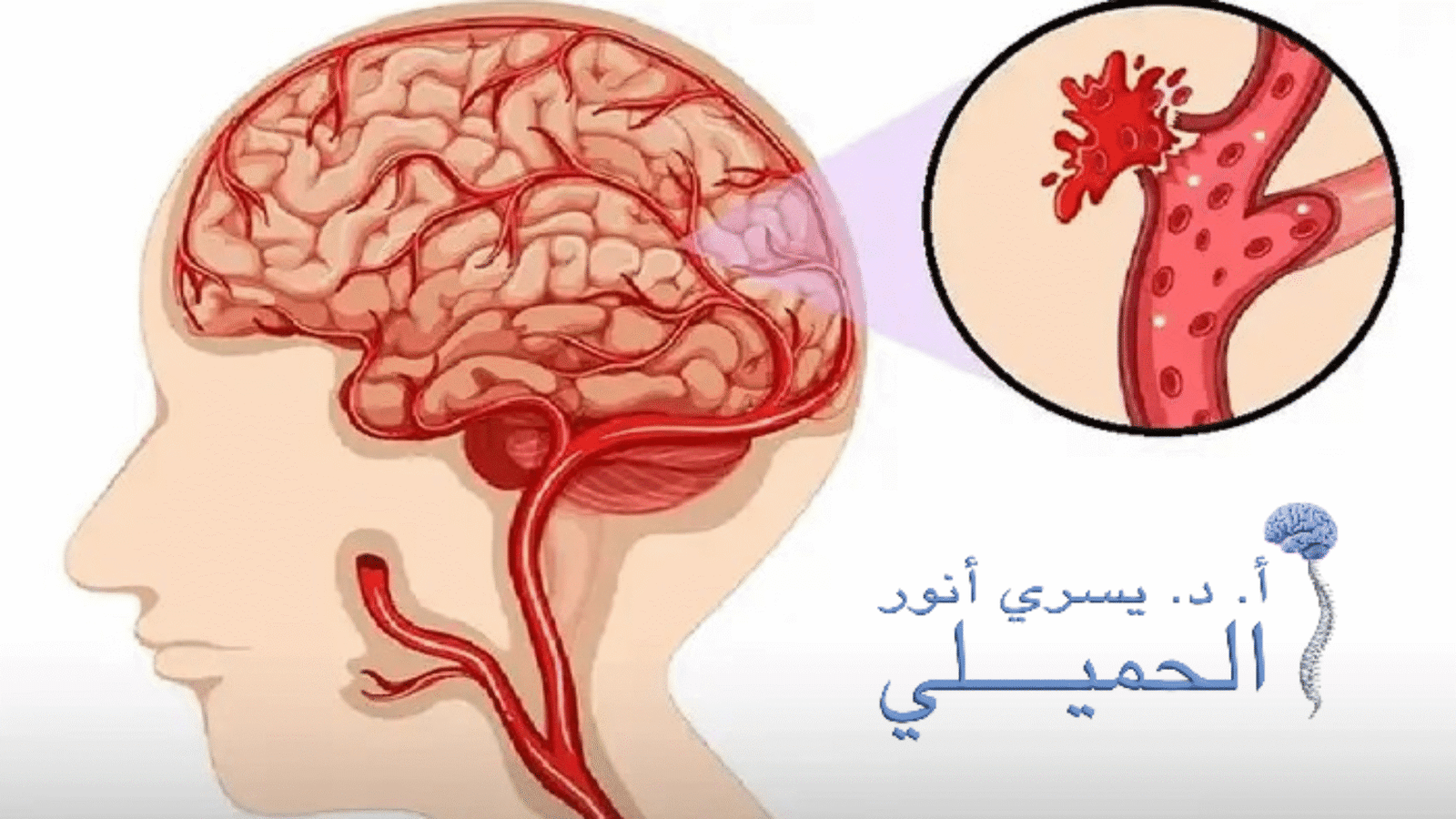
A brain hemorrhage is a form of stroke that occurs when blood vessels in the brain rupture, often due to a sudden rise in blood pressure. This leads to blood leaking into brain tissue, reducing blood flow and nutrient supply to affected areas and limiting oxygen delivery essential for normal brain cell function. As a result, brain cells may gradually die, and in some cases, the condition can progress to partial or complete paralysis if not treated urgently or if complications are not controlled in time.
Causes:
Several factors can lead to a brain hemorrhage, and identifying the exact cause often guides treatment decisions. The most common causes include:
-
Chronic high blood pressure: Continuous pressure weakens blood vessel walls and increases the risk of rupture.
-
Head injuries and trauma: Falls or traffic accidents can cause intracranial bleeding, particularly in children and young adults.
-
Aneurysms: Weakness in brain artery walls may lead to rupture and internal bleeding.
-
Congenital vascular malformations: Such as arteriovenous malformations (AVMs), where blood vessels are more prone to bleeding from birth.
-
Brain tumors: Some tumors, especially malignant ones, may cause bleeding due to pressure on blood vessels or vessel rupture.
-
Blood and clotting disorders: Low platelet counts or clotting disorders increase bleeding risk.
-
Chronic diseases: Conditions such as diabetes, heart disease, and atherosclerosis affect blood vessel health.
-
Lifestyle factors: Smoking, alcohol consumption, and drug abuse weaken blood vessels.
-
Pregnancy and childbirth complications: Conditions such as preeclampsia or the effects of certain contraceptives may increase hemorrhage risk.
-
Blocked brain arteries or clots: Arterial blockage can raise pressure and cause blood leakage.
Can Brain Hemorrhage Be Cured?
The possibility of recovery depends on multiple factors related to the patient’s condition and the severity of the hemorrhage. In some cases, full recovery is achievable, while in others, long-term complications affecting brain function may remain. The earlier the medical intervention and the more limited the brain tissue damage, the higher the chances of recovery.
Factors Affecting Recovery:
-
Location of the hemorrhage: Bleeding near vital brain areas makes recovery more challenging.
-
Size of the hemorrhage: Larger hemorrhages increase the likelihood of permanent brain damage.
-
Speed of medical intervention: Early diagnosis and prompt treatment significantly improve recovery chances.
-
Overall health condition: Patients with chronic illnesses may face greater recovery challenges.
Treatment Options:
Types of Treatment for Brain Hemorrhage
Treatment depends on the size and location of the hemorrhage and the patient’s condition:
1. Medical Treatment:
-
Medications to lower blood pressure.
-
Drugs to control brain swelling and prevent complications.
2. Surgical Treatment:
-
Removal of accumulated blood to relieve pressure on the brain.
-
Repair of damaged blood vessels.
-
Use of endoscopic techniques to minimize surgical intervention.
3. Rehabilitation After Hemorrhage:
-
Physical therapy to improve movement and balance.
-
Occupational therapy to support daily activities.
-
Psychological support to manage stress and anxiety.
4. Supportive Care:
-
Close medical follow-up to prevent complications and ensure treatment effectiveness.
Is Full Recovery Possible After a Brain Hemorrhage?
This depends on each patient’s individual condition. Some patients may return to their normal lives after full recovery, while others may experience long-term effects such as difficulty with movement, speech, or concentration. In such cases, physical and psychological rehabilitation becomes essential to improve daily functioning and adapt to post-hemorrhage challenges.
How Is Brain Hemorrhage Diagnosed?
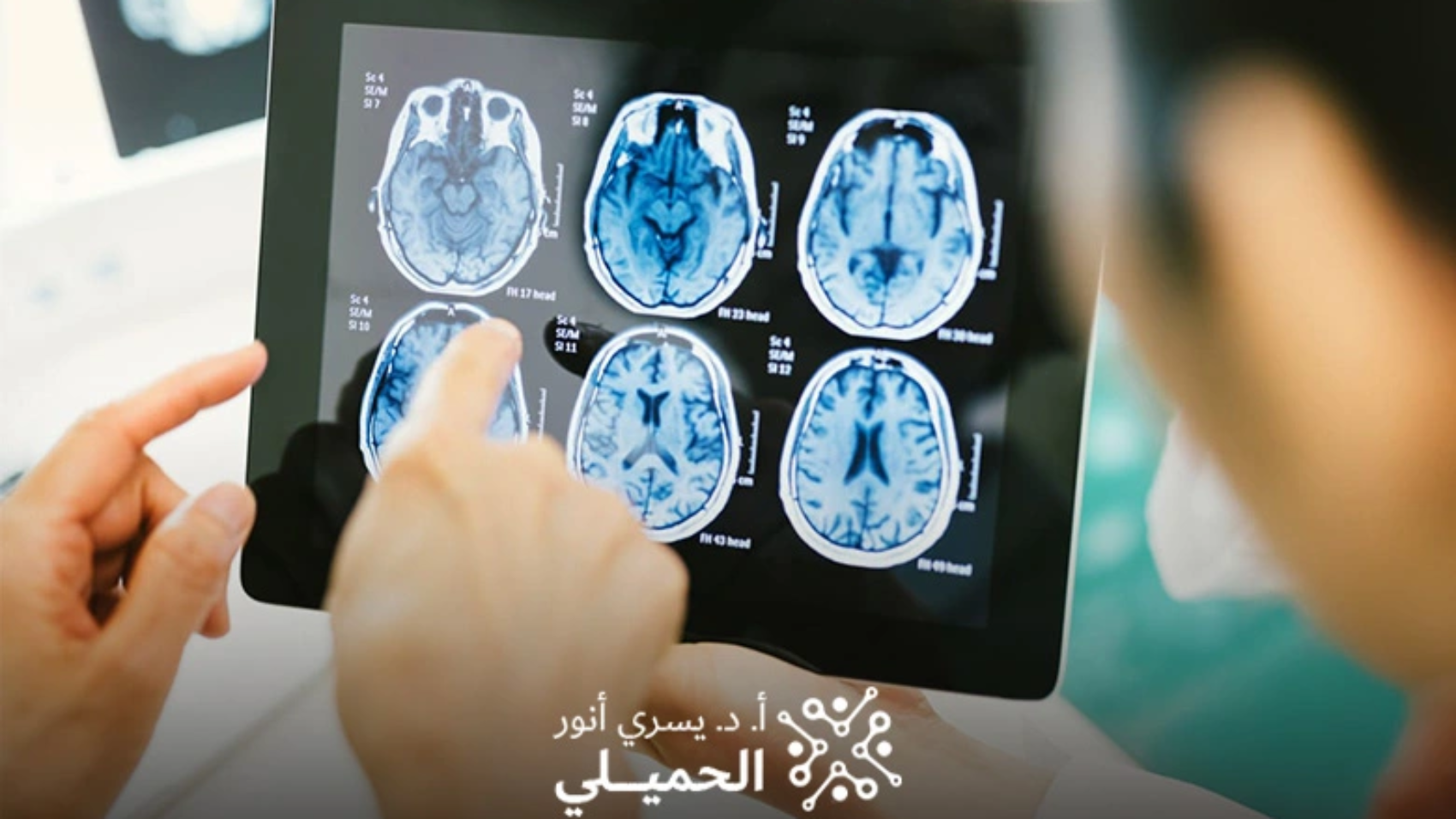
Severe brain injuries are medical emergencies that require rapid assessment and treatment. The physician examines the patient and asks key questions, such as whether a head injury occurred, the specific symptoms experienced, whether the patient lost consciousness, and for how long. Based on this information, the doctor determines the location and size of the hemorrhage and conducts diagnostic tests, including:
-
CT scan of the brain
-
MRI of the brain
How Can Brain Hemorrhage Be Prevented?
The risk of brain hemorrhage can be reduced by following simple and effective measures, including:
-
Monitoring blood pressure: Keeping blood pressure within normal ranges reduces vessel rupture risk.
-
Preventing injuries: Using safety equipment during sports or driving to avoid head trauma.
-
Quitting smoking: Smoking increases blood vessel fragility.
-
Following a healthy diet: Balanced nutrition supports cardiovascular and vascular health.
When Should You Consult a Brain Hemorrhage Specialist?
If you need specialized medical advice regarding brain hemorrhage and its aftereffects, Dr. Yousri Al-Hamili is considered one of the leading specialists in neurosurgery, offering expertise in managing brain hemorrhage cases and guidance on neurological care after bleeding.
You should seek immediate medical attention if any of the following symptoms appear:
-
Sudden, severe headache unlike usual headaches
-
Weakness or numbness in one side of the body
-
Difficulty speaking or seeing
-
Loss of consciousness or decreased alertness
Early diagnosis and rapid intervention play a crucial role in reducing the risk of serious complications and improving recovery outcomes.
Conclusion
Recovery from a brain hemorrhage depends on the speed of medical intervention, the type of hemorrhage, and the patient’s overall health. Some patients achieve full recovery, while others may require long-term follow-up to manage lasting effects. Adherence to treatment plans and regular follow-up with specialized physicians are key to achieving the best possible outcomes.
Frequently Asked Questions (FAQ)
1. Can brain hemorrhage be cured?
Yes, recovery from a brain hemorrhage is possible in many cases, especially with early medical intervention and an appropriate treatment plan. Recovery depends on the size and location of the hemorrhage, treatment speed, and the patient’s overall health. Some patients fully recover, while others may need long-term rehabilitation.
2. What are the main causes of brain hemorrhage?
Causes include chronic high blood pressure, head injuries, aneurysms, vascular malformations, brain tumors, blood clotting disorders, chronic diseases such as diabetes and heart disease, as well as smoking, alcohol use, and drug abuse.
3. How is brain hemorrhage treated?
Treatment depends on the severity and location of the hemorrhage and the patient’s condition. It may include medications to control blood pressure and swelling, surgical intervention to remove accumulated blood and repair vessels, and rehabilitation programs such as physical and occupational therapy along with psychological support to enhance recovery.